 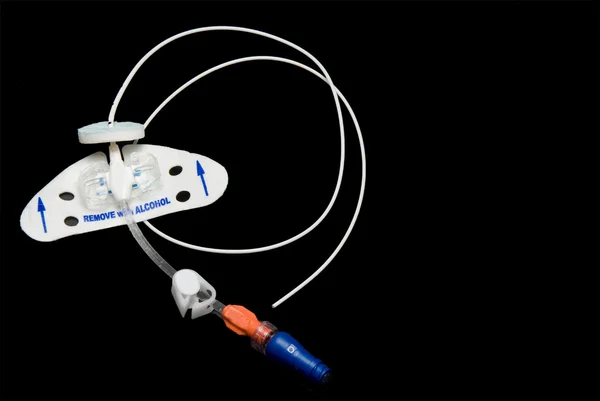 
In addition to arterial injury, peripheral nerves and brachial nerve plexuses present in the upper extremity may be damaged. Vascular complications such as accidental arterial puncture, bleeding, vasospasm, and pseudoaneurysm formation have been reported in the literature following PICC insertion. The most common complications tend to be vascular in nature. PICCs are generally inserted safely, but complications may arise relating to device insertion, functionality, or post-procedure infection. After each use, the PICC should be flushed with normal saline. Dressings should be changed at a minimum once per week. The dressing and venotomy site should be inspected to check for bleeding and erythema. 
Secure the catheter to the skin using a locking device and cover it with dressings. Remove the obturator and place caps on the PICC lumens. Aspirate and flush each lumen checking for blood return. Snap open and pull the two wings of the sheath apart and alternate advancing catheter between pulls slightly. Slowly insert the entire length of PICC with obturator into the introducer sheath and visualize with fluoroscopy correct positioning at the cavoatrial junction. Place a finger over the opening of the introducer to avoid air aspiration during removal. Remove the wire and dilator while leaving the introducer in place. Trim the catheter to the previously measured length using the scalpel provided in the PICC kit. Thread the introducer and dilator over the wire, through the skin, and into the vein. Using the scalpel, make a small nick in the skin to widen the needle tract to allow more room for the introducer. Remove the needle while keeping the wire in place. Advance guidewire through the needle and check wire purchase with fluoroscopy to ensure positioning in at minimum the subclavian vein. An axial view of the vessel with the ultrasound will allow visualization of the needle tip. Ultrasound will confirm the correct positioning of the needle within the vein, as will blood return from the needle. Using the access needle, puncture the vein while directly visualizing the needle tip. Sedation may be given for the procedure.ĭirectly visualize the access vein with ultrasound and anesthetize the skin and subcutaneous tissue over the area of the vein with 1% lidocaine. Flush all catheter lumens with normal saline and clamp them shut. Ensure items are in the center of the sterile field. Ensure supplies are arranged in a sterile and organized fashion for easy access. Place the sterile cover over the ultrasound probe. Appropriately drape the patient with sterile draping material. Prep the area with an antiseptic solution. This will be the approximate measurement of the catheter. With the measuring tape, measure the distance from the antecubital fossa to the midclavicular line and turn the tape measure to reach the third intercostal space at the right border of the sternum. Use ultrasound to identify and select the appropriate vessel for access. Place the patient in a supine position with the arm abducted and externally rotated. Connect the patient to a cardiac monitor to detect arrhythmias that may occur as a result of wire access into the right atrium. If the venous system of the right upper extremity is not accessible due to superficial infection, trauma, or obstruction, a left-sided approach may be attempted.ĭiscuss the procedural risks and benefits with the patient. Alternatively, the cephalic vein may be used for access. There is a higher risk of inadvertent arterial puncture with this venous access location with the brachial artery nearby. If the basilic vein is not accessible or occluded, an attempt at accessing the right brachial vein may be attempted. It is thought that this vein also has the least number of valves and provides a more optimal access angle. A right basilic venotomy location provides the least tortuous path toward the superior vena cava. The right and left innominate veins to combine at the superior vena cava. After combining with the brachial vein, the axillary vein is formed, which becomes the subclavian vein at the border of the first rib and continues centrally to become the brachiocephalic (innominate) vein. Originating from the dorsal venous network of the hand, the basilic vein travels on the medial aspect of the upper extremity. The basilic vein is usually accessed between the axilla and the antecubital fossa. The right basilic vein’s size and proximity to the skin make it the attempted vein of choice for PICC placement. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
